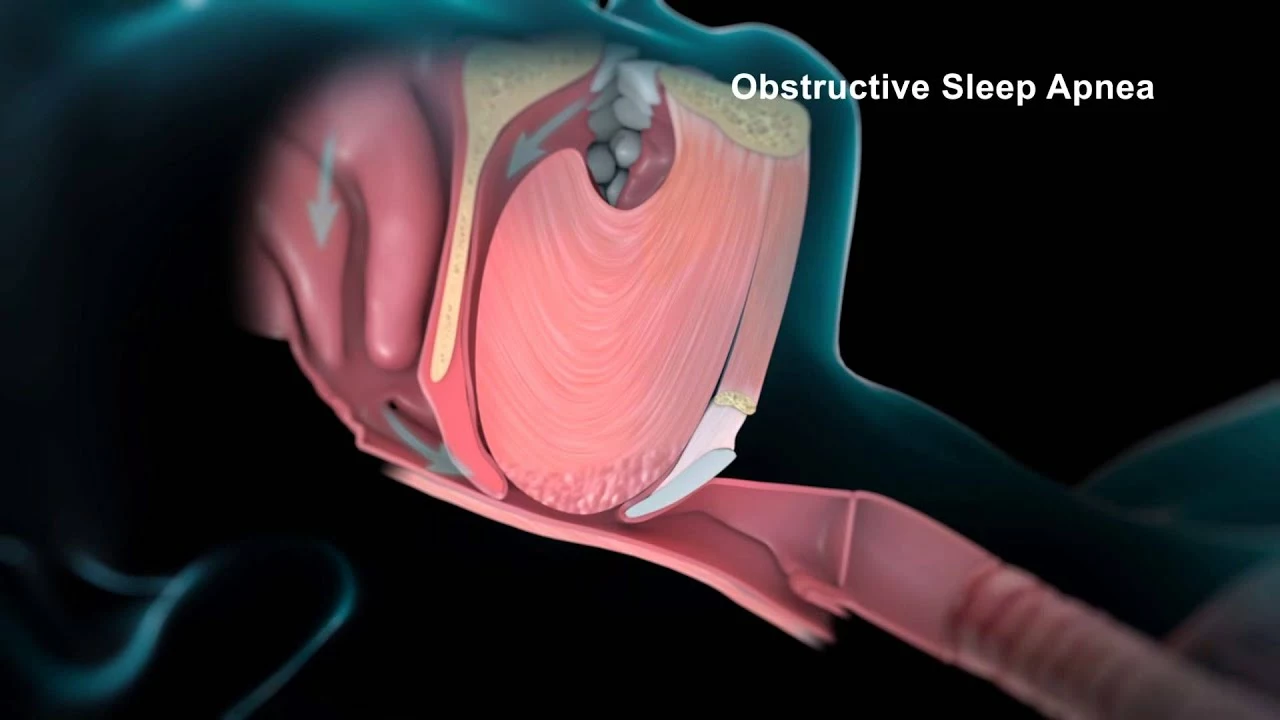
Sleep Apnea: Spot Symptoms, Get Tested, and Start Feeling Better
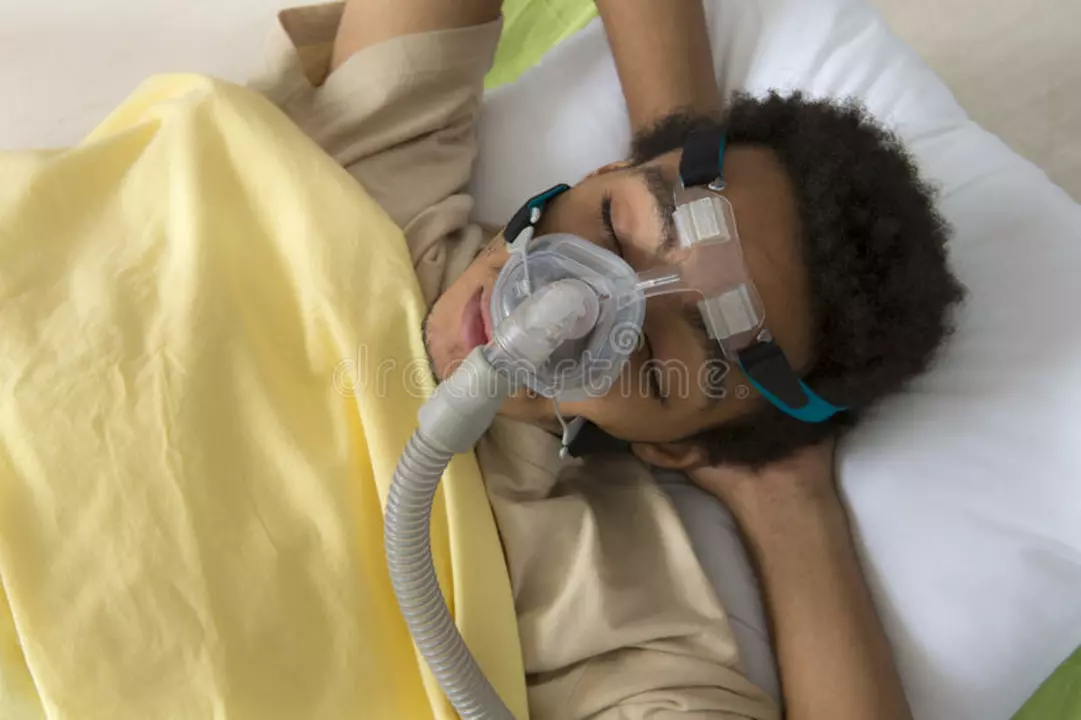
Do you wake up tired even after a full night’s sleep? Loud snoring, choking, or gasping during sleep are common signs of sleep apnea. This isn’t just annoying — untreated sleep apnea raises blood pressure, tires you out, and can increase heart and stroke risk. The good news: many effective, practical fixes exist, and you don’t have to guess which one fits you.
Symptoms and when to get tested
Look for these red flags: loud, habitual snoring; witnessed pauses in breathing; morning headaches; daytime sleepiness that affects work or driving; trouble concentrating. If a bed partner reports pauses or gasps, see a doctor. Primary care docs often start with a sleep questionnaire and may refer you for a sleep study. Home sleep apnea tests work well for straightforward cases and measure breathing and oxygen levels overnight. If your case is complex, a lab-based polysomnography gives a fuller picture.
Treatment options and how to pick gear safely
First-line treatment for moderate to severe obstructive sleep apnea is CPAP (continuous positive airway pressure). It forces air into your airway to stop collapses. A few practical tips: get a mask that fits — nasal or full-face — because a leaky mask ruins sleep. Use a humidifier if your nose gets dry. Ask your provider to fine-tune pressure or try an auto-adjusting CPAP so the machine finds the right pressure each night.
For mild cases or if you can’t tolerate CPAP, a mandibular advancement device (an oral appliance) can push the lower jaw forward to keep the airway open. Have a dentist trained in sleep medicine fit it; off-the-shelf mouthguards rarely work well. Positional therapy (avoiding back sleeping) helps some people. Weight loss, quitting smoking, and cutting alcohol before bed reduce symptoms for many.
When you buy devices online, follow safety steps: buy from reputable suppliers, confirm the product is FDA-cleared or CE-marked, keep prescriptions handy if required, check return and warranty policies, and read recent reviews. Avoid super-cheap, unbranded CPAPs and masks — poor fit and bad seals lead to worse sleep and skin problems.
Cleaning matters: wipe the mask daily, wash cushions and tubing weekly with mild soap, and replace filters and parts on the schedule the manufacturer recommends. Proper care avoids mold, skin irritation, and machine failure.
If CPAP and oral devices don’t help, talk to an ENT or sleep surgeon about nasal surgery, palate procedures, or implant options. Always treat sleep apnea — it’s more than snoring. Getting tested and using the right treatment will boost daytime energy, improve mood, and protect your heart.
Still unsure where to start? Ask your primary care doctor for a sleep referral. A quick screening test and a home study can get you a clear plan within weeks, not months.